Game on, age off: physical activity and virtual reality in older adults
Physical inactivity affects approximately 1.4 billion people worldwide – around one quarter of the global population – and is particularly prevalent among adults aged 60 and over. Many individuals in this age bracket fail to achieve the recommended 150 minutes of moderate-to-vigorous physical activity (PA) per week [1, 2]. This sedentary pattern accelerates declines in physical performance, cognitive function, and overall health, while intensifying age-related concerns such as fall risk, chronic disease, and social isolation [3, 4]. Regular PA offers neuroprotective benefits and may lower the risk of neurological conditions such as dementia and Alzheimer’s disease [5]. As the global population ages, innovative, multidimensional interventions have become increasingly urgent [6].
Immersive virtual reality (VR) has emerged as a promising approach. By delivering interactive, sensorimotor-rich environments, VR can counter both physical inactivity and social disconnection in older adults [7, 8]. Head-mounted displays (HMDs), including devices such as the Oculus Quest, HTC Vive, and Meta Quest 2, immerse users in 360-degree environments that stimulate physical, cognitive, and social engagement.
These systems enhance motivation through gamification, instant feedback, and goal-based challenges. At the neurocognitive level, VR activates attentional and sensorimotor circuits using ecologically valid, multisensory simulations that require dynamic body movement [8–10]. This combination fosters neuroplasticity by engaging physical and cognitive functions simultaneously, promoting gains in executive function, visuospatial skills, and working memory [11, 12]. Adaptive feedback systems also adjust in real time to user performance, supporting personalised learning curves [13]. VR may therefore play a key role in fostering autonomy in ageing [9, 10, 14].
Despite its potential, VR adoption among older adults remains limited. Challenges include low digital literacy, physical discomfort, safety concerns, and a shortage of age-specific content. Calibration complexity and interface design can further reduce usability and adherence in geriatric settings [14–16].
VR is often used as a broad term in the literature, encompassing semi-immersive tools like the Microsoft Kinect or Nintendo Wii. This review adopts a narrower scope, focusing solely on immersive VR systems using HMDs and motion tracking to create spatially interactive, multisensory environments. Unlike non-immersive devices, immersive VR incorporates gesture tracking, haptic feedback, and full-body interaction. While VR can replicate real-world scenarios [17, 18], further research is needed to assess the long-term impacts on physical, cognitive, and emotional health [8].
Recent studies suggest VR can significantly enhance exercise adherence and balance, particularly for fall prevention [14, 19, 20]. VR also shows promise in supporting cognitive function across neurodegenerative conditions, offering an engaging and flexible platform for stimulation [4, 21, 22]. Together, these findings highlight VR’s therapeutic value in producing integrated physical and cognitive benefits.
The integration of VR into digital health marks a paradigm shift in how PA is conceptualised, moving beyond static metrics to include full-body, sensor-driven interactions. In rehabilitation, this now encompasses activities beyond traditional sedentary formats, such as virtual cycling, that yield substantial energy expenditure[8].
Activities are often categorised by metabolic equivalents (METs); exercises exceeding 1.5 METs, such as virtual boxing or cycling, are linked to cardiovascular improvement and reduced mortality [23, 24]. However, the lack of standardised metrics across VR systems remains a methodological challenge[8].
A rigorous narrative review is needed to consolidate this growing body of evidence, map key trends, and identify ongoing limitations [25]. This review aims to examine immersive VR-based motor interventions targeting older adults. Specifically, we (1) distinguish immersive VR from other digital modalities; (2) identify the key factors influencing intervention effectiveness, including usability and engagement; and (3) highlight successful implementations and persistent gaps. By uniting insights across disciplines, this review offers a framework for future research and the ethical integration of VR into geriatric care and public health.
In doing so, it also poses a deeper question: does the rise of immersive VR signal a new paradigm in ageing care or echo Icarus, ascending brilliantly yet blindly towards an indifferent sun? In this context, ‘Icarus New Rising’ gestures less towards cautionary collapse than towards the paradox of technological elevation – at once luminous and uncertain – that defines the contemporary ageing experience.
Setting the stage: literature search strategy
This narrative review follows a methodologically transparent synthesis, explicitly guided by the SANRA (Scale for the Quality Assessment of Narrative Review Articles) framework to ensure analytical depth and scientific rigour. Aligned with SANRA’s first criterion – justification of relevance – this work addresses a timely and underexplored question: how immersive VR may mitigate motor and cognitive decline in older adults. The second criterion – clear articulation of aims – is met through three objectives: (1) distinguish immersive VR from other digital tools; (2) examine its multidimensional health effects; and (3) identify barriers to broader implementation.
The third criterion – transparent search strategy – is satisfied through a structured search conducted across PubMed, Web of Science, ScienceDirect, and Scopus. Boolean logic was applied across three thematic domains: technology, motor intervention, and ageing (see Table 1). All records were imported into EndNote X9, and duplicates were removed automatically before screening. Manual screening of reference lists complemented the database search.
Table 1
Search strategy in scientific databases
The fourth criterion – appropriate referencing – is addressed through an interdisciplinary bibliography that includes clinical trials, systematic reviews, and conceptual work in gerontology, neuropsychology, rehabilitation, and digital health. Although no formal appraisal tool was used, study limitations, including small samples and methodological inconsistency, are critically acknowledged throughout.
The fifth SANRA criterion – balanced presentation of evidence – is reflected in our thematic structure: physical, cognitive, emotional, and social domains are analysed with transparency, clearly separating robust findings from preliminary trends. Methodological heterogeneity is consistently flagged. Thus, the SANRA framework is not merely cited but substantively enacted, reinforcing both the scientific integrity and translational relevance of this review.
The search strategy was developed using predefined Boolean combinations of terms from three conceptual domains: (a) immersive technology (e.g., ‘virtual environment’, ‘augmented reality’); (b) motor intervention (e.g., ‘physical therapy’, ‘movement-based therapy’); and (c) participant characteristics (e.g., ‘older adults’, ‘geriatrics’). Within-domain terms were linked with ‘OR’, and domains combined using ‘AND’. The full syntax appears in Table 1. Reference lists of included studies were also screened manually.
Two independent reviewers screened all titles, abstracts, and full texts for eligibility. Disagreements were resolved by consensus. Eligible study designs included randomised controlled trials (RCTs), and quasi-experimental, observational, and mixed-methods studies, capturing the field’s methodological diversity. This dual review process reduced selection bias and ensured consistency.
Studies were included only if the motor interventions were delivered exclusively via immersive VR platforms. Eligible interventions had to provide a multi-sensory, spatial experience capable of inducing presence. Only HMDs (e.g., Oculus Quest, HTC Vive) offering panoramic views and engaging cognitive faculties met inclusion. Semi- or non-immersive systems – such as Kinect, Nintendo Wii, or Cave Automatic Virtual Environments (CAVE) – were excluded due to their lower sensory and spatial interactivity.
To ensure relevance, we limited inclusion to peer-reviewed studies published in English between 2017 and 2024 – a period marking the emergence of clinically viable immersive VR systems. While this language restriction may introduce bias, it is justified by the dominance of English in digital-health publishing and the lack of consistent multilingual indexing.
Conference abstracts, proceedings, and unpublished manuscripts were excluded. Because this review synthesises existing literature, no new data were collected. All included studies adhered to the ethical standards reported by their authors and institutions, and no additional ethical approval was required.
To synthesise the evidence base, we developed a tabular synopsis of studies meeting the inclusion criteria. These investigations span diverse methodological designs ranging from randomised controlled trials to feasibility and user-centred studies and focus exclusively on immersive VR interventions delivered via HMDs. Table 2 (see end of paper) summarises each study’s design, technology, duration, population characteristics, and key outcomes. Collectively, this synthesis maps the landscape of immersive VR-based motor interventions in older adults while illuminating the consistencies and innovations that guide the subsequent analysis.
Table 2
Summary of immersive VR motor-intervention studies included in this review (2017–2024)
| Author(s) and year | Design | VR type | Duration | Population | Conclusions |
|---|---|---|---|---|---|
| Appel et al. (2020) [39] | mixed methods | Samsung Gear VR HMD | 3–20 min of 360°-video footage of nature scenes | 66 older adults (mean age 80.5, SD = 10.5) | It is feasible and safe to expose older adults with various levels of cognitive and physical impairments to immersive VR within these settings |
| Barsasella et al. (2021) [19] | RCT | HTC Vive | 6 weeks, 2×/ week, 15 min/ session | 60 older adults (29 IG: 4M/25F; 31 CG: 10M/21F); community-dwelling; mean age not reported | VR sessions have the potential to influence the well-being and functional fitness of older adults and further support the process of healthy and active ageing |
| Béraud-Peigné et al. (2024) [42] | RCT (pilot) | immersive and interactive wall exergames (I2WE) | bi-weekly one-hour group sessions over 12 weeks (24 sessions) | 34 older adults; mean age ~70; 19 IG (I2WE), 15 CG (Walking & Muscle Training) | Improved visuospatial working memory, inhibition, dual-task performance (IG only); improved all physical functions except upper body strength (both groups); improved perceived pleasure in I2WE group |
| Campo-Prieto et al. (2022) [45] | RCT (pilot) | HTC Vive Pro | 10 weeks, 3×/week, 6 min/session | 12 nonagenarian women; EG (n = 6; 91.7 ± 1.6), CG (n = 6; 90.83 ± 2.6); community-dwelling; Spain | Improved balance (Tinetti test: balance +10.97%, total +10.2%); improved usability (SUS = 78.3); no dropouts; no cybersickness; maintained TUG times; effective and well-accepted IVR intervention |
| Campo-Prieto et al. (2022) [10] | RCT | HTC Vive Pro | 10 weeks, 3×/week, 6 min/session | 24 older adults (13 EG, 11 CG); mean age ~85; mixed sex | Improved balance, gait, handgrip (EG); no drop-outs; high adherence |
| Campo-Prieto et al. (2022) [32] | feasibility study | HMD Oculus Quest 2 | 60 sessions, short duration | 32 Parkinson’s disease patients; mean age 71.5 ± 11.8; 78% men; Spain | The use of the FIT-XR exergame in the PD population and position the Oculus Quest 2 HMD as a suit-able wearable device for physical activity and with which to carry out future rehabilitation programs |
| Campo-Prieto et al. (2021) [61] | feasibility study | HTC Vive Pro | 2 sessions (~10–12 min each, separate days) | 4 healthy older men; aged 65–77; no previous gaming experience | High usability (SUS > 85); no cybersickness; im-proved satisfaction; improved motivation; positive physical engagement; feasibility of IVR for older adults during the COVID-19 pandemic using commercial HMDs |
| Chaze et al. (2022) [53] | mixed-methods (pilot) | Oculus Rift VR technology | ~2 weeks, 8–10 min/session | 32 older adults in LTC homes, mean age = 77, SD = 10.64; 47% female | Improved well-being across physical (less pain, move-ment), cognitive (memory), emotional (joy, calm) and social (engagement with staff/peers) domains |
| Drazich et al. (2023) [55] | RCT (pilot) | fully immersive VR (Holofit via Oculus Quest) | 8 weeks, 2×/week, 40 min sessions | 20 older adults (10 VR, 10 control); aged 55; urban independent living facility; diverse (63% black); mean age 74 | Feasible, safe (no cybersickness), high adherence (15/16 sessions avg.), improved vigorous PA in VR group, high acceptability and appropriateness reported, potential to reduce depressive symptoms though not significant |
| Høeg et al. (2023) [17] | feasibil-ity study (mixed-methods) | Pico G2 4K VR headsets | 2×/week, 15–20 min | 10 hospitalised older adults (mean age 80.3, 50% women) | High acceptability and feasibility, promoted feel-ings of autonomy and competence |
| Høeg et al. (2023) [14] | mixed methods | Collaborative IVR tandem biking (social scenario, HMD) | ~10.7 min/ session with a mean speed of 14.8 km/h (± 5.8) | 11 older outpatients; 64% male; mean age 60 | Improved usability (score 85/100), improved enjoyment, improved motivation, improved relatedness, reduced VR sickness, collaborative tasks well-received, time distortion observed |
| Huang et al. (2020) [46] | repeated measures design | IVR exergaming (Fruit Ninja VR, Oculus Rift) | 4 weeks, 2×/week, 20 min/session | 33 adults (mean age = 61.93, SD = 8.21; female = 24); randomised to immersive vs. non-immersive | Immersive experience of exergaming would elicit the feeling of presence, which later contributes to improved cognitive performance in inhibition and task switching |
| Kim et al. (2017) [16] | pre-post intervention study | Oculus Rift Development Kit 2 | 5 min bouts on treadmill, 20 min/session | 11 healthy young adults (28 ±7 years), 11 healthy older adults (66±3 years), and 11 individuals with Parkinson’s disease (65 ± 7 years) | 20 min of walking in an immersive environment using the Oculus Rift did not induce simulator-related sickness or alterations in static or dynamic postural control |
| Kruse et al. (2021) [41] | mixed-methods | Maestro Game VR (custom immersive exergame, Valve Index HMD) vs. 2D exercise video | 1 session (7–10 min VR); rest and counter-balanced conditions | 25 older adults (mean age 81.24 ± 4.97; 3M, 22F); all living independently; Germany | VR exergame was perceived as enjoyable and novel, but the 2D video was preferred for long-term use due to higher physical demand and familiarity. VR offered more feedback and adjustability, but less variety of movement. Both scored similarly on enjoyment, attention, and workload; heart rate was higher for video. VR seen more as a ‘game’ than ‘exercise’ by some |
| Kwan et al. (2021) [48] | RCT (pilot) | Immersive VR (HTC Vive Focus Plus) with cognitive game + cycling ergometer | 8 weeks, 2×/week, 30 min/session | 17 community-dwelling older adults with cognitive frailty; median age 74; Hong Kong | VR simultaneous motor-cognitive training is effective at enhancing the cognitive function of older people with cognitive frailty. VR training is feasible and safe for older people with cognitive frailty |
| Liao et al. (2019) [49] | RCT (single-blinded) | VR (Kinect-based) with IADL-based physical and cognitive tasks | 12 weeks, 3×/week, 60 min/session | 34 older adults with mild cognitive impairment; community-dwelling; Taipei, Taiwan | Significant improvements in dual-task gait performance in older adults with mild cognitive impairment, which may be attributed to improvements in executive function |
| Liao et al. (2020) [40] | RCT (single-blinded) | Kinect + HTC Vive (custom IADL-based VR) | 12 weeks | Older adults with mild cognitive impairment; Taipei, Taiwan | VR-based physical and cognitive training improves cognitive function, instrumental activities of daily living and neural efficiency in older adults with mild cognitive impairment |
| Lima Rebêlo et al. (2021) [20] | RCT | Oculus Rift; HMD | 16 sessions, 2×/week; 50-minute morning sessions | 37 older adults (aged 60–79) with balance disorders and fall risk; 20 IVR, 17 control | Immersive VR training effective for balance-related outcomes, although it was not superior to conventional therapy |
| Lin and Wu (2021) [57] | between-subjects experiment | HTC Vive HMD; embodiment of avatars (young vs. old) | one VR-based exercise session (brief acclimation, guided workout, and voluntary practice) + next- day follow-up call | 104 older adults (60–88 yrs; mean = 70.4); 51 older-avatar (26F/25M), 53 young-avatar (27F/26M); did not engage in vigorous PA; Taiwan | Embodiment of younger avatars increased perceived exertion during exercise, especially among female participants. Findings support the Proteus effect in older adults; avatar age influenced motivation and exercise effort |
| Micarelli et al. (2019) [50] | RCT | home-based immersive VR (HMD) for vestibular rehab | twice a week for 4 weeks for 30–45 min | 47 older adults with unilateral vestibular hypofunction (UVH), with or without mild cognitive impairment | The implementation of a home-based VR protocol may be a safe option in order to improve vestibu- lo-ocular reflex, postural control and the quality of life also in the vestibular impaired patients in whom the presence of cognitive decline could hin- der the achievement of the goal of rehabilitation |
| Muhla et al. (2020) [29] | comparative within-subject design | HTC Vive (HMD) | 2 conditions (TUG real vs TUG VR), 3 trials each | 31 older adults (mean age 73.7 ± 9), 20F/11M, post-rehabilitation, community-dwelling | The mean completion times and most of the mean number of steps of the Timed Up and Go in the VR condition were significantly different to those in the clinical condition. These results suggest that there is a VR effect, and this effect is significantly correlated to the time taken to complete the Timed Up and Go |
| Muñoz et al. (2022) [47] | user- centred design (multi-stakeholder) | HMD-VR (Oculus Quest 1 & 2); exergame Seas the Day | 15 min/ session (warm-up, conditioning, cooldown) | 5 exercise professionals, 5 community-dwelling older adults, a VR company for content creation, and a multidisciplinary research team with game designers, engineers, and kinesiology experts | The process provide a replicable model of interaction that blends the needs and preferences of end users with those of exercise providers |
| Phu et al. (2019) [30] | pre- and post-intervention study | BRU – Balance Rehabilitation Unit | 6 weeks, 2×/week, 30 min/session | 195 older adults (median age 78, IQR 73–84); 63 BRU, 82 EX, 50 controls; 67% female; community-dwelling, high risk of falls | Potential use of VR as a practical alternative to improve outcomes of balance training for reduction of falls risk in older adults |
| Sakhare et al. (2019) [34] | feasibility study | Immersive VR (HTC Vive Pro); stationary bike with spatial navigation | 10–12 min total: 4 task trials (2–3 min) | 40 adults (20 younger, 25.9 ± 3.7 yrs; 20 older, 63.6 ± 5.6 yrs); community-dwelling, cognitively healthy | Spatial navigation while cycling is feasible and older adults report similar experiences to younger adults. VR may be a powerful tool for engaging physical and cognitive activity in older adults with acceptable adverse effects and with reports of en- joyment |
| Stamm et al. (2022) [31] | randomised controlled pilot study | Immersive VR (HTC Vive); ViRST exergame with movement and psychoeducation | 4 weeks; 3×/week, 30 min/ session | 22 older adults ( 65 years) with chronic back pain; IG = 11, CG = 11 | VR therapy led to improved functional capacity and was well rated in user experience; pain reduc- tion was lower than the control group but feasible as an adjunct therapy |
Ageing gracefully with VR: a look at its multidimensional impacts
In the digital age, VR is increasingly recognised as a promising tool to support multiple facets of healthy ageing. Far beyond its entertainment appeal, VR enables immersive, meaningful experiences – from exploring Machu Picchu to participating in virtual yoga – that encourage PA, cognitive engagement, emotional balance, and social connection. As such, it emerges not merely as a novelty, but as a holistic platform for autonomy and sustained participation in later life[9].
Although often associated with gaming, VR has deep roots in domains such as military training, aviation, and clinical rehabilitation, where its immersive and interactive nature enhances skill acquisition and therapeutic outcomes[26]. Over the last decade, VR has evolved into a versatile health technology with growing relevance in geriatric care. Systematic reviews now highlight its benefits across key areas, including balance improvement, cognitive stimulation, pain modulation, and social engagement[9, 27, 28]. These findings suggest that VR can play a vital role in improving quality of life and promoting positive behavioural change in ageing populations[29].
To explore these multidimensional effects, the following subsections examine how immersive VR contributes to four interrelated pillars of healthy ageing: physical function, cognitive vitality, emotional well-being, and social connectedness.
Enhancing physical health and function through immersive exercise
Immersive VR, delivered through HMDs, is increasingly recognised as a valuable tool in geriatric health and rehabilitation. By combining PA with multisensory, interactive environments, VR enhances accessibility and motivation, particularly for older adults with mobility limitations [30, 31]. It complements rather than replaces traditional methods, offering structured and adaptive opportunities for movement.
This subsection explores four key domains of physical health that benefit from immersive VR: balance and fall risk, muscular strength and mobility, pain management, and long-term engagement (motivation and adherence).
Balance and fall risk
Exergames that simulate sports, dance, or movement-based challenges have shown considerable efficacy in improving balance and reducing fall risk among older adults [14, 19, 20]. Designed to be both engaging and safe, these interventions address many of the motivational and logistical barriers that often limit participation in traditional exercise programs [14].
Protocols that incorporate real-time visual feedback often outperform conventional training by enhancing functional mobility, postural control, and both static and dynamic balance [17]. Home-based applications, such as virtual cycling or rhythm games (e.g., Beat Saber), extend accessibility and are particularly suitable for individuals with restricted mobility [21].
VR’s ability to support postural alignment and core stability adds another therapeutic layer. Simulations that prompt real-time adjustments through visual and haptic feedback improve proprioceptive awareness, which is essential for individuals at higher risk of falls due to postural or gait impairments [32].
However, outcomes vary. Older adults with higher baseline mobility tend to show faster and more pronounced gains, while those with greater physical limitations may require slower-paced, customised protocols. This variability underscores the need to calibrate the intensity and progression to individual capacities [27, 28].
HMD-based interventions can significantly enhance performance on standard clinical assessments, including single-leg stance, sit-to-stand tests, Timed Up and Go (TUG), Four Square Step Test, and gait speed evaluations [29, 30]. These improvements reinforce VR’s potential role in fall prevention and functional rehabilitation.
Importantly, beyond physical metrics, VR has been shown to reduce the fear of falling – a psychological barrier that often deters older adults from staying active. A 10-week immersive exergaming program evaluated by Campo-Prieto et al. [10] demonstrated marked improvements in balance, mobility, and functional strength, including handgrip – a reliable predictor of independence in ageing populations.
Strength and mobility
In addition to balance, immersive VR interventions have demonstrated positive effects on muscular strength, especially in the core and lower extremities, which are essential for maintaining independence and preventing frailty in later life. Exercise programs that incorporate resistance-based tasks, such as virtual squats, lunges, or strength-focused activities, have been linked to measurable gains in endurance and functional performance [31].
Repetitive, guided movements in VR scenarios contribute to improved flexibility, joint mobility, and reduced stiffness [9, 32]. These physical adaptations translate into better performance in daily activities, such as stair climbing, rising from a chair, or reaching overhead, reinforcing autonomy and confidence [32].
Pain management
Chronic pain remains a widespread barrier to PA among older adults. VR offers a novel approach by using immersive distraction to reduce perceived discomfort during movement. This cognitive-affective mechanism allows users to shift their focus away from pain, making exercise more tolerable and even enjoyable [33].
By reframing the sensory experience, VR can increase pain thresholds and promote adherence to therapeutic regimens. In this context, immersive VR serves not only as a motivational tool but also as a complementary strategy in pain management, particularly within movement-based interventions.
Sustaining engagement and promoting adherence
One of VR’s most compelling advantages lies in its ability to sustain long-term engagement in exercise – a challenge in traditional programs often seen as monotonous or exhausting. The gamified architecture of immersive platforms, featuring real-time feedback, progressive challenges, and reward systems, transforms PA into an experience that feels both motivating and personally meaningful.
That said, extended or unsupervised VR use may cause adverse effects, including cybersickness, eye strain, disorientation, or dizziness, particularly among individuals with limited experience in digital environments [34, 35]. These symptoms, although typically temporary, can erode confidence and limit sustained use.
Mitigation strategies include optimised frame rates, user-controlled navigation, gradual exposure, and shorter session durations. Equally critical is the development of intuitive, age-appropriate interfaces and onboarding procedures. Personalised technical support further reduces cognitive load and fosters a sense of digital mastery. Research shows that when these supports are in place, older adults not only participate more regularly but also report greater satisfaction and self-efficacy in maintaining physical health through VR [36].
Limitations and future directions
Despite encouraging results, several limitations still constrain both the scientific validity and real-world adoption of VR interventions for older adults. A primary concern is the prevalence of small sample sizes, which limits statistical power and reduces generalis-ability [32]. Many studies also evaluate interventions lasting only a few weeks, leaving the durability of the gains uncertain.
Methodological heterogeneity represents another critical barrier. Variations in hardware, exercise intensity, and outcome measures make it difficult to compare studies or establish standardised best practices. The inclusion of non-immersive platforms further muddies comparisons, as these systems lack the sensory richness of fully immersive VR. This inconsistency also leads to underreporting of potential side effects such as cybersickness [36, 37].
To advance the field, future research must prioritise larger, more diverse samples and adopt consistent, validated protocols. Harmonising intervention designs and outcome metrics will support robust meta-analyses and help establish evidence-based clinical guidelines.
There is also a need to determine the optimal ‘dose’ of VR – including frequency, duration, intensity, and progression – tailored to individual functional profiles. Adaptive algorithms that dynamically adjust challenge levels may prove especially effective in sustaining engagement and maximising benefit.
Stratified analyses are essential to understand how VR interventions affect specific subpopulations, such as individuals with frailty, vestibular dysfunction, or mild cognitive impairment. Tailoring interventions to these clinical profiles will likely enhance both safety and therapeutic efficacy, increasing the chances of successful implementation in real-world care settings [17, 38].
To synthesise current findings, Table 3 below summarises the most common types of VR exercise and their associated physical outcomes in older adults.
Table 3
Overview of VR exercise types and their associated physical outcomes in older adults
In summary, immersive VR shows strong potential to enhance physical health in older adults, with growing evidence of benefits across balance, muscular strength, mobility, and pain management. These improvements contribute meaningfully to two pillars of healthy ageing: autonomy and fall prevention. However, to fully realise this potential, interventions must be personalised to individual functional baselines and evaluated through trials with standardised protocols, validated outcome measures, and sufficient statistical power. Achieving this will require not only technological refinement and inclusive design but also a robust, high-quality evidence base, grounded in clinical diversity and real-world settings [18, 19, 38].
Among physical outcomes, balance and gait performance are the most consistently improved, with moderate effect sizes reported across several pilot studies and small RCTs. Still, the underlying evidence remains heterogeneous in design, duration, and outcome assessment. Most studies rely on small samples and short interventions and lack long-term follow-up, limiting both generalisability and insight into sustained impact. Therefore, these findings should be interpreted with caution, particularly regarding their clinical applicability.
Cognitive gains through dual-task integration
VR is increasingly redefining intervention models in geriatric health by combining PA with cognitive stimulation on a single, synergistic platform [39, 40]. Moving beyond its recreational origins, immersive VR has demonstrated the potential to enhance executive function and cognitive flexibility through simulations that activate motor and cognitive systems simultaneously [41–43].
VR-based interventions support not only cognitive health but also physical performance, including improved balance, mobility, and functional capacity. This dual-action approach positions VR as a powerful complement to traditional therapies, with the capacity to promote multidimensional health in older adults [10, 34].
One of the most promising applications of VR lies in dementia care, where immersive exergames have been shown to support both cognitive integrity and physical engagement [44]. These dual-task platforms are gaining traction as innovative therapeutic tools [45, 46] capable of slowing decline and sustaining motivation across the neurocognitive spectrum [4, 21, 22]. Interdisciplinary efforts are now focused on developing tailored VR solutions that integrate advanced sensors, enabling highly personalised environments that promote both neurocognitive stimulation and motor learning [8, 14, 47].
Across the literature, key cognitive outcomes include improved task-switching, stronger inhibitory control, and increased dual-task gait speed – all markers of enhanced executive function [21, 46, 48]. These gains are frequently attributed to paradigms requiring users to engage motor and cognitive faculties simultaneously, thereby strengthening cognitive-motor integration in ecologically valid contexts.
For instance, Liao et al. [49] showed that VR-based gait training significantly improved both executive functioning and gait in older adults with mild cognitive impairment. These findings highlight the interdependence between motor and cognitive domains and the therapeutic potential of dual-task VR interventions [48].
VR has also shown promise in vestibular rehabilitation, improving balance control, cognitive function, and vestibulo-ocular reflex gains in individuals with unilateral vestibular hypofunction, even in those with concurrent cognitive impairments [50]. This suggests that VR can recalibrate postural strategies and reduce fall risk through multisensory training [51].
Recent advances include adaptive VR systems that automatically adjust task difficulty and walking speed based on user performance. These dynamic environments are particularly relevant for individuals with motor-cognitive disorders such as Parkinson’s disease [15] and open up new avenues for biomechanical monitoring and motor-control research.
Emerging studies also point to a bidirectional relationship between cognition and motor function. VR-based cognitive-motor interventions targeting daily-living skills have been linked to improvements in coordination, divided attention, and cognitive flexibility – all critical for maintaining independence [49]. However, much remains unknown. Future research must identify which cognitive subdomains are most responsive to VR and determine the optimal frequency, duration, and complexity of interventions.
Sustained interdisciplinary collaboration is essential to refine protocols, improve usability, and clarify the neurophysiological mechanisms underlying the observed gains [36, 37, 51]. In parallel, rigorous validation studies are needed to evaluate efficacy, safety, and feasibility across diverse populations, paying special attention to headset ergonomics, session length, and instructional clarity, all of which influence user comfort and cognitive load [51].
Neuroimaging work further underscores the cognitive potential of immersive VR. Functional magnetic resonance imaging (MRI) studies reveal task-specific activation and cortical reorganisation consistent with enhanced cognitive functioning after VR interventions [52]. These data suggest that VR is not merely a delivery channel but a transformative modality capable of engaging the brain in novel and potent ways.
As a convergence point among cognitive science, rehabilitation, and gerontology, VR offers a new paradigm for integrated care. Its ability to engage physical and mental faculties simultaneously holds great promise for cognitive resilience and functional autonomy. Yet this promise remains provisional unless supported by robust, standardised research. When grounded in rigorous design and person-centred principles, immersive VR can serve not just as a cognitive training tool, but as a platform for holistic and dignified ageing.
Among cognitive outcomes, the most consistent findings involve improvements in executive function, attention, and dual-task performance, particularly in older adults with mild cognitive impairment. Nevertheless, most evidence stems from pilot or proof-of-concept trials with small samples, brief durations, and heterogeneous protocols. The absence of validated cognitive batteries, the inconsistent outcome measures, and the undefined dose–response relationships further complicate the evidence base. Without standardised metrics, stratified sampling, and long-term follow-up, claims about VR’s cognitive benefits will remain suggestive rather than conclusive.
Feel-good factor: psychological and emotional well-being
Immersive VR is increasingly viewed as an effective avenue for supporting the psychological and emotional well-being of older adults. Beyond traditional therapies, VR creates immersive environments that offer both digital escapism and affective stimulation – relieving stress, elevating mood, and fostering emotional engagement. In one study, Barsasella et al. [19] found that exposure to calming virtual landscapes significantly reduced symptoms of anxiety and depression, while increasing a sense of presence and emotional connection.
These environments can function both as emotional refuges and as invitations to movement – especially through interactive, nature-based simulations. In this way, VR disrupts the sedentary routines common in later life, encouraging embodied interaction in restorative, digitally mediated settings [34]. This fusion of immersive technology and biophilic design signals a shift in mental-health care, reimagining how therapeutic engagement can occur in ageing populations [53, 54].
While research is still emerging, early findings suggest that VR is feasible, acceptable, and well tolerated. In a pilot study, Drazich et al. [55] reported moderate effects on depressive symptoms in older adults, especially those at higher psychological risk. Though limited by small samples and low baseline distress, the study confirmed that immersive interventions were safe, engaging, and positively received.
VR does not only mitigate negative emotional states; it also promotes positive psychological outcomes such as increased self-esteem and greater motivation for PA [33, 56]. Through real-time feedback, goal-oriented tasks, and accessible scenarios, VR can create a sense of progress and mastery – key drivers of self-efficacy, particularly among adults with limited prior engagement in structured exercise.
Emerging research on the Proteus effect – the idea that users’ self-perception shifts according to their avatar – offers further insight. Lin and Wu [57] showed that avatar embodiment in exercise contexts significantly influenced motivation and affective experience in older users. These findings highlight avatar design not merely as a technical detail but as a powerful psychological lever in personalised health promotion.
Social connection also plays a central role in emotional well-being and sustained engagement. Høeg et al. [14] examined social interaction in a VR ‘buddy biking’ game, where participants reported greater emotional involvement and enjoyment when activities were shared. Expressive avatars and synchronised tasks enhanced interaction quality and perceived connection – although limitations in avatar realism still posed barriers to deeper emotional exchange.
Together, these studies suggest that VR may help address affective needs in ageing populations. Documented benefits include mood enhancement, reduced anxiety and depressive symptoms, increased confidence, and higher motivation for movement. Still, to move beyond feasibility, VR must be integrated with broader strategies – including social support, physical rehabilitation, and community-based initiatives.
Nonetheless, several challenges remain. Issues of accessibility, digital safety, and emotional appropriateness must be addressed. Barriers such as cost, limited digital literacy, cybersickness, and discomfort with hardware still hinder widespread adoption [58]. Ensuring inclusive use will require age-friendly interfaces, simplified onboarding, and ongoing technical support.
Ethical concerns – particularly around privacy, consent, and emotional vulnerability – must also be taken seriously as VR becomes more integrated into mental-health care [59]. Transparent data practices, clear informed-consent procedures, and built-in emotional safeguards should be embedded into both design and delivery.
While immersive VR holds early promise for enhancing psychological resilience and improving quality of life, the evidence remains preliminary. Reported improvements in mood and motivation tend to be modest and inconsistent, and are often drawn from pilot studies with small samples, brief exposures, and limited control conditions. Moreover, effects may be influenced by novelty, short-term emotional uplift, and user expectations – factors rarely tracked over time. Without longitudinal data, it remains unclear whether VR’s emotional benefits are sustainable, clinically meaningful, or best suited as adjuncts to broader interventions.
To establish a credible role for VR in emotional care, future studies must adopt robust designs with standardised affective measures, stratified recruitment, and extended follow-up periods. Only then can we determine whether VR is best deployed as a preventive tool, a therapeutic supplement, or a short-term motivational enhancer. With continued interdisciplinary collaboration, ethical design, and inclusive implementation, immersive VR may become a core component of holistic ageing care – integrating physical vitality with emotional depth and social presence.
Social connections and quality of life
As social isolation becomes a pressing challenge in ageing societies, VR offers a novel and potentially powerful solution for [restoring] and enriching interpersonal connections. Platforms like Alcove VR, Meta Quest 2, and EngageVR create immersive social environments where older adults can engage in shared activities, maintain relationships, and form new ones – often overcoming the physical and geographic barriers that limit face-to-face interaction [38, 54, 59]. These virtual experiences range from collaborative games to cultural exploration, collectively promoting a sense of community and reducing loneliness.
Beyond mere connection, VR is evolving into a medium for meaningful, sustained social engagement. In a study by Høeg et al. [14], participants in a VR cycling game reported greater emotional involvement and enjoyment when challenges were undertaken collaboratively. Real-time communication during scenic virtual rides helped (re-create) genuine social dynamics, even in the absence of physical presence. These experiences suggest that VR can support emotionally rich interactions and reframe digital spaces as sites of community and shared meaning. Nevertheless, the same study also noted technological limitations: avatar expressiveness and gesture nuance remain insufficient for conveying complex social cues, (sometimes) limiting the depth of connection and highlighting the need for more emotionally intelligent design features.
Another promising feature of VR is its ability to facilitate purposeful digital escapism. Far from being merely distracting, VR can transport older adults to emotionally significant spaces, such as a childhood neighbourhood, a world-class museum, or a cherished seasonal festival. These simulations can rekindle autobiographical memory, evoke affective resonance, and reinforce a sense of identity, agency, and continuity in later life [43, 60].
To fully leverage this potential, future research must explore the specific social needs and preferences of older adults, including the desire for authentic, emotionally resonant interactions. Longitudinal studies are essential to assess the durability of virtual relationships, their impact on offline social integration, and their role in intergenerational connection – for example, playing VR games with grandchildren. Features that support shared goals, such as team-based challenges, progress tracking, and cooperative rewards, may also enhance motivation and deepen social ties [35].
Yet these possibilities must be balanced against practical and ethical concerns. Barriers to access persist: many older adults face limited digital literacy, hardware discomfort, and skepticism about technology. Addressing these issues will require inclusive design principles, simplified user interfaces, ergonomic hardware, and reliable technical support [58, 59]. Without such accommodations, VR may inadvertently deepen digital exclusion, especially among those it aims to serve.
Moreover, most current studies on social VR benefits rely on small, non-representative samples and short-term interventions. While some report reductions in loneliness and increased connectedness, these findings are often drawn from brief exposures, with limited attention to sustainability, relational depth, or translation to real-world outcomes. Critically, the experience of social presence – essential to VR’s relational success – is highly sensitive to variables like avatar realism, response latency, and environmental stability. These elements are seldom reported or standardised, making it difficult to compare findings or develop best practices.
To build a solid foundation, future research must employ validated interactional metrics, stratify participant characteristics, and assess whether virtual relationships contribute to tangible improvements in offline well-being. Studies should also distinguish between passive co-presence and active engagement, and investigate how virtual social bonds evolve over time. Until such evidence is available, the role of VR in addressing social isolation must be considered promising yet preliminary – a tool with clear potential, but not yet an established therapeutic modality.
To summarise the multidimensional benefits of immersive VR for older adults, Table 4 offers a synthesised overview of impacts across the physical, cognitive, emotional, and social domains.
Table 4
Summary of the impacts of VR on older adults by domain
While immersive VR offers compelling opportunities to support healthy ageing, current empirical evidence remains uneven across domains. Physical outcomes show the strongest support, with several small-scale trials reporting moderate short-term gains in balance, strength, and mobility. In contrast, cognitive, emotional, and social findings are still drawn largely from pilot work with methodological variability and brief durations.
Across all areas, the field lacks standardised outcome measures, consistent intervention taxonomies, and robust comparisons with conventional care. To move beyond promise, future investigations must employ adequately powered multisite trials and incorporate cost-effectiveness analyses. Stratified sampling and extended follow-up will be essential to evaluate the long-term sustainability, equitable access, and real-world applicability. Only through this level of methodological consolidation can immersive VR become a credible, scalable tool in geriatric care.
If successful, VR may not only support rehabilitation but also help realise a broader vision of ageing – one that is active, participatory, and digitally inclusive. Ultimately, the promise of immersive VR lies not in the technology itself, but in how we choose to shape it around the needs, dignity, and lived experiences of the older adults it is meant to serve.
A digital leap: promises and pitfalls of VR in geriatric care
Immersive VR represents a paradigm shift in geriatric care, offering older adults immersive environments where physical limitations are transcended and new forms of engagement, learning, and social connection become possible. By expanding access to wellness activities and interpersonal experiences, VR is positioned not merely as a tool but as a transformative medium for promoting autonomy and quality of life, regardless of geography or physical ability. This section critically examines both the potential and the barriers to sustainable VR integration in ageing care.
Promises: engagement, adherence, and well-being
Growing evidence supports the efficacy of immersive VR – particularly HMDs – in promoting PA among older adults [10, 45, 48]. Studies report improvements in balance, mobility, and motivation for sustained engagement [34]. In a study by Syed-Abdul et al. [35], older adults responded positively to VR, citing ease of use, perceived benefits, and enjoyment as key motivators for adoption. Similarly, Campo-Prieto et al. [61] found high user satisfaction, reinforcing the idea that positive affect and intrinsic motivation – the ‘fun factor’ – are critical for adherence.
This success is increasingly driven by interdisciplinary collaboration. Muñoz et al. [47] emphasise the importance of user-centred design and continuous feedback, especially in dementia care, where emotional resonance is pivotal. Drazich et al. [55] further demonstrate that immersive VR interventions are both feasible and acceptable in ageing populations, with strong potential to support moderate-to-vigorous activity and enhance psychological outcomes.
By aligning therapeutic goals with immersive engagement, VR introduces a novel framework for holistic geriatric wellness [16, 50]. Gamifying health behaviours transforms repetitive tasks into meaningful, personalised experiences, fostering both adherence and empowerment [34]. Low dropout rates across studies indicate that well-designed VR interventions can support the long-term preservation of cognitive and physical function [21].
Pitfalls: barriers to widespread adoption
Despite promising results, significant obstacles hinder broad VR integration in geriatric care. These include technological unfamiliarity, high costs, health-related concerns, and broader ethical and regulatory gaps [15, 16].
A critical issue involves the collection and storage of biometric and behavioural data – gaze, physiology, in-app actions. Older users may be especially vulnerable to data misuse or breaches. Ethical deployment demands end-to-end encryption, transparent consent protocols, and data-minimisation practices that prioritise autonomy and control [59].
Interface complexity also deters adoption. Many systems feel unintuitive, with complicated controls, disorienting calibration, or abstract navigation [34, 56]. Solutions include voice-guided menus, streamlined user flows, and age-adapted onboarding. Peer-led training and community tech hubs can further build confidence.
Financial barriers are substantial, particularly for adults on fixed incomes. Potential remedies include subsidies for medically approved devices, insurance reimbursement models, and the development of low-cost standalone systems [62]. Public access points, such as libraries, clinics, and non-governmental organisations, can bridge gaps in underserved areas.
Offline content, ergonomic design, and simple interfaces are also essential for scalability and inclusion. Ultimately, successful implementation depends on participatory design models and institutional support frameworks that promote sustained use and contextual flexibility [63, 64].
Another challenge is cybersickness – dizziness, nausea, or disorientation from sensory mismatch. Although some evidence suggests older adults may be less susceptible [16, 48, 55], user comfort remains paramount. Strategies include shorter sessions, smoother motion, user-controlled pacing, and gradual exposure [14, 65]. Future research should further investigate age-related physiological responses to VR, including baseline assessments and tailored exposure regimens [55].
Finally, there are structural gaps in workforce readiness and regulation. Few training pathways exist for clinicians, and regulators have yet to define clear criteria for certifying immersive VR as a clinical modality.
Overcoming these barriers will require multifaceted action that integrates inclusive design, evidence-based development, and institutional support. Only then can VR evolve from a promising innovation into a scalable, trusted pillar of geriatric care.
Pathways toward equitable integration
Beyond the technical and ethical dimensions, integrating VR into geriatric care demands attention to sociocultural and relational factors. While immersive technologies can foster inclusion by enabling shared virtual experiences, they also risk deepening social disconnection if used as substitutes – rather than complements – to real-world interaction. VR should be framed not as a replacement for embodied relationships, but as a tool that expands participation for individuals facing mobility or geographic constraints [53, 54].
Cross-sector collaboration is essential. Clinicians, developers, policymakers, and older adults themselves must engage in co-design processes that yield systems that are both technologically advanced and socially relevant. Inclusive design practices rooted in user diversity and cultural sensitivity align VR applications with the realities, preferences, and capabilities of ageing populations.
Healthcare integration must honour autonomy, dignity, and person-centred care. Interventions should be tailored to individual goals while respecting cognitive thresholds, emotional readiness, and physical limitations. In this context, VR becomes more than a therapeutic modality – it serves as a platform for meaningful engagement, helping older adults reclaim agency and connection in daily life.
In summary, VR holds significant promise as a catalyst for healthy, empowered ageing – enhancing physical function, cognitive resilience, and emotional well-being. Yet realising this potential hinges on overcoming systemic barriers through inclusive innovation, collaborative design, and sustained ethical reflection. When developed with care and implemented equitably, immersive VR can mature into a cornerstone of agefriendly digital-health ecosystems that fosters not only health but also dignity, participation, and connection across diverse older populations [14, 47].
What about the future? A virtual leap forward
The integration of VR into geriatric care continues to open up promising pathways for improving older adults’ well-being by addressing longstanding barriers such as accessibility, affordability, and personalisation. To fully harness this potential, targeted strategies, including subsidy programs, insurance coverage, and partnerships with community and healthcare organisations, are essential to ensure equitable access to immersive technologies at low or no cost [16, 35]. Parallel to this, ongoing research is critical to address the specific needs of ageing populations, focusing on digital literacy, usability, and self-efficacy [66, 67].
Role of technology: personalised and predictive interventions
A particularly exciting frontier lies in the convergence of VR and artificial intelligence (AI). AI systems can enable real-time adaptation and predictive analytics, dynamically personalising VR-based rehabilitation. By detecting subtle movement patterns, AI-driven platforms can automatically adjust task intensity, refine feedback, and tailor content continuously [68, 69]. This supports not only responsiveness but also preventive care, reducing injury risk and enhancing intervention efficacy.
Future studies should explore how AI can integrate multimodal physiological and behavioural data, such as heart rate variability, gait metrics, and fatigue indicators, to support precision rehabilitation. Predictive models could help clinicians tailor interventions to individual profiles, anticipating plateaus, regressions, and emerging risks [69].
Complementing this, VR’s integration with the Internet of Things (IoT) is creating intelligent, connected rehabilitation ecosystems. Wearable and embedded sensors, like smart insoles, accelerometers, and heart rate monitors, allow real-time tracking of exertion, posture, and motor control [70]. For example, if biometric signals indicate fatigue or cardiovascular stress, the system can immediately lower task demands or initiate rest intervals, enhancing both safety and autonomy.
Augmented Reality (AR) adds another dimension to this evolving landscape. Unlike VR, which immerses users in fully virtual settings, AR overlays digital cues onto physical environments, enabling hybrid simulations. Older adults can rehearse daily tasks, such as cooking or crossing a street, in familiar yet digitally enhanced settings. These ecologically valid scenarios improve engagement and facilitate the transfer of learning to real-world activities [8, 69]. When embedded within exergames, the combination of AR and VR creates multisensory, emotionally engaging experiences that blend physical effort, cognitive challenge, and social interaction. This multifaceted stimulation may enhance adherence and long-term behavioural change, especially when the interventions are personalised and socially meaningful [69].
Building a supportive ecosystem: from technology to community
Technological progress must be matched by the creation of robust social and structural ecosystems. Community-based initiatives, such as VR clubs, peer mentoring, and intergenerational programs, can foster adoption and reduce the technological apprehension common among older adults.
To succeed, these systems must be developed through transdisciplinary collaboration. Involving gerontologists, engineers, clinicians, and policymakers ensures that accessibility, ethical principles, and inclusivity are embedded from interface design to clinical deployment. Such partnerships promote not only functional usability but also cultural and cognitive relevance, aligning VR tools with the diverse realities of ageing.
Research frontiers: addressing gaps and limitations
Despite encouraging outcomes, current research remains early-stage and methodologically inconsistent. Trials vary widely in design, sample size, duration, and outcomes [60], limiting the generalisability and comparison. Methodological refinement is needed across four domains: standardised assessment protocols to enable comparability; longitudinal studies to assess sustained effects; contextual analyses, especially in low-resource or rural settings; and systematic monitoring of adverse effects, including cybersickness, fatigue, and emotional strain.
The long-term viability of VR depends not only on its clinical effectiveness but also on its scalability across healthcare systems. Future studies should address cost-effectiveness, workforce training, and integration into public health infrastructures, particularly where VR could supplement gaps in conventional care [63, 64].
New advances in motion capture and biometric sensing open the door to even more tailored interventions. These technologies can measure posture, gait variability, movement symmetry, and reaction time in three-dimensional space. Additionally, biometric signals like heart rate, skin conductance, or pupillometry can infer emotional state and cognitive load, allowing real-time adjustments in task complexity [43, 71, 72].
Inclusiveness demands interfaces designed for diverse physical and cognitive capacities. Multimodal systems – voice commands, eye tracking, gesture recognition – must be coupled with adaptive pacing and layered feedback, giving users autonomy over their engagement. Just as crucial is evaluating the subjective user experience, including motivation, enjoyment, frustration, and fatigue, which remains underexplored but essential to long-term success [73].
Integrating behavioural science models, such as the Technology Acceptance Model and the Behaviour Change Support System, can enhance both adoption and adherence [73–76]. These frameworks emphasise ease of use, perceived value, and intuitive design as key predictors of engagement [74].
Effective strategies should include gradual onboarding with low cognitive load, clear feedback loops and adaptive challenges, and social reinforcement such as peer recognition and cooperative tasks. Together, these elements support sustained participation in VR-based physical and cognitive programs. Combining user-centred design with behavioural modelling and mixed-methods evaluation offers a strong foundation for accessible, engaging, and scalable VR for healthy ageing [73].
To synthesise the evolving role of VR in geriatric care, Table 5 contrasts current applications with emerging innovations across six critical domains, outlining a trajectory from foundational use to transformative integration:
Table 5
From today to tomorrow: the evolution of VR for older adults
As the digital landscape evolves, VR is shifting from an auxiliary tool to a central pillar of equitable ageing. Achieving this vision requires applications that are inclusive, adaptive, and responsive to the heterogeneity of older populations – particularly those with limited mobility, health vulnerabilities, or low digital literacy.
Crucially, the promise of VR lies not only in its therapeutic utility but in its transformative capacity to reimagine ageing itself. Rather than reinforcing narratives of decline, immersive technologies can empower older adults as agents of their own well-being, active participants in virtual communities, and contributors to new cultural imaginaries of ageing.
Sustained investment in inclusive design, cross-disciplinary collaboration [77], and behavioural insight will be essential. Only then can VR realise its full potential as a catalyst for autonomy, dignity, and meaningful engagement in later life.
The final frontier: new horizons in ageing
This review underscores the transformative potential of immersive VR in reshaping geriatric care. By introducing scalable, multisensory tools, VR offers novel ways to enhance autonomy, engagement, and well-being in later life. As global populations age, the urgency for holistic and innovative strategies intensifies – strategies capable of addressing the interconnected challenges of physical decline, cognitive deterioration, emotional vulnerability, and social isolation. Through sensorimotor-rich, emotionally resonant environments, VR emerges as a multidimensional intervention that promotes PA, stimulates cognition, fosters emotional resilience, and cultivates meaningful social connection.
Empirical evidence increasingly supports VR’s positive impact on ageing. Studies have shown that VR can significantly improve physical outcomes, such as balance and muscular strength, thereby reducing fall risk, a leading cause of morbidity in older adults. Cognitive benefits have also been observed, particularly in memory, attention, and executive functioning, offering promise for delaying age-related decline. Emotionally, VR appears to reduce anxiety and depressive symptoms while enhancing self-esteem and affective engagement. Socially, it facilitates geographically unbounded interaction, offering new avenues for combating loneliness and exclusion.
Still, important limitations remain. Much of the current research lacks methodological consistency, making it difficult to disentangle VR’s specific effects from those of other interventions. The absence of stand-ardised outcome measures, especially in the cognitive and emotional domains, undermines comparability across studies. Small sample sizes, short intervention periods, and heterogeneous participant cohorts further constrain generalisability. Systemic barriers, such as low digital literacy, high equipment costs, and inadequate infrastructure, continue to impede the broader adoption of VR in geriatric care.
To address these challenges, future research must adopt interdisciplinary and translational approaches, bridging biomechanics, cognitive neuroscience, ger-ontology, and behavioural science. For instance, the integration of motion capture technologies with neuropsychological testing could enable the design of VR scenarios that simultaneously target postural stability and cognitive engagement. Likewise, individualised psychological profiling could inform content personalisation, adapting experiences to emotional thresholds, attentional bandwidth, and motivational patterns.
Collaboration is paramount. Clinicians, designers, engineers, and policymakers must co-develop VR interventions that are not only scalable and clinically relevant but also ethically sound and responsive to real-world conditions.
Concrete implementation steps are now required. These include integrating VR into primary care and rehabilitation pathways, training healthcare professionals in both facilitation and ethical deployment, and developing standardised implementation protocols that detail session frequency, duration, and follow-up to guide routine clinical use. In the digital age, VR represents more than a therapeutic innovation; it signifies a conceptual shift in how ageing is understood, experienced, and enacted.
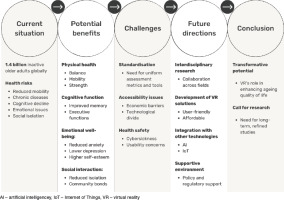
Figure 1 illustrates the multidimensional impacts of VR on physical, cognitive, emotional, and social health in older adults.
Looking forward, research should prioritise large-scale longitudinal studies with rigorous designs. These studies must include systematic monitoring of adverse effects, such as cybersickness, cognitive fatigue, and sensory overload, and explicitly differentiate immersive from non-immersive systems to clarify their effectiveness and inform evidence-based guidelines. Equally essential is the development of validated frameworks and standardised implementation protocols, which are foundational for both clinical integration and policy adoption.
The successful integration of VR into geriatric care will hinge on sustained, interdisciplinary cooperation. Technologists, healthcare providers, and researchers must ensure that VR tools are not only effective and scalable but also accessible, culturally relevant, and adaptable to the physical and cognitive diversity of ageing populations.
To guarantee equitable access, digital health initiatives for older adults must be treated as public goods. This will require investments in infrastructure, the creation of public–private partnerships, and alignment with international goals for active and dignified ageing. VR must not remain confined to elite systems but be embedded in universal strategies for health equity.
At the same time, ethical foresight must be embedded across all stages – from design to deployment. An ‘ethics by design’ approach grounded in transparency, autonomy, inclusivity, and non-maleficence is essential to protect vulnerable users and build public trust in digital therapeutics. Participatory design frameworks are likewise crucial: older adults must be engaged not merely as end-users, but as active co-creators of the very technologies intended for their benefit. Such engagement ensures that interventions are not only ethically robust but also socially grounded and contextually meaningful.
By refining strategies and dismantling systemic barriers, VR can evolve from a promising enhancement into a foundational element of integrated geriatric care. In doing so, it may help redefine ageing itself – not as a trajectory of decline, but as a co-authored space of innovation, where dignity, agency, and digital equity shape futures worth inhabiting.